
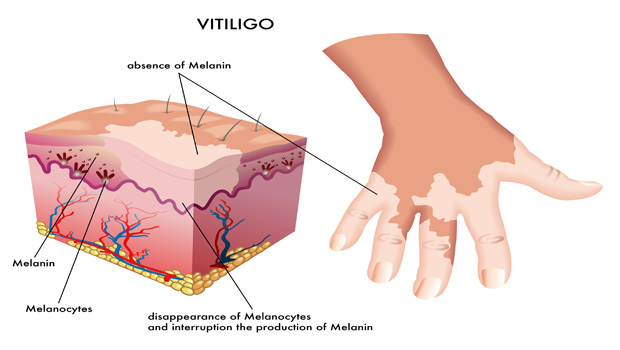
Vitiligo is a disorder of pigmentation in which skin starts losing its original color leaving white discolored patches on the skin. It can occur at any age and visibility of patches is greater in people with dark skin tone. It can affect any skin area of the body and the hair and lips.
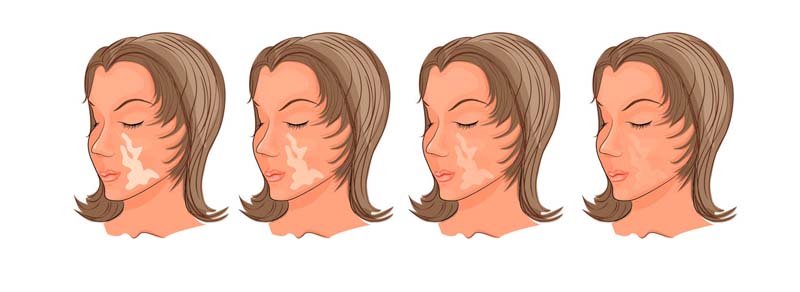
Treatment :
There are various treatment options including topical creams (steroids, tacrolimus, calcipotriol, prostaglandins), light therapy, photo-chemotherapy, oral drugs (steroids, immunomodulators, antioxidants) and surgery.
Vitiligo Surgery:
Surgical treatment is an option in those patients who have not responded to adequate trial of medical therapy and their disease is stable. Stable disease means no new lesions have appeared and existing lesions have not increased in size during last one year.
Skin Grafting:It is useful for the small patches of vitiligo. Thin layers of healthy skin are removed from the donor site on the patient’s body using fine instruments and attached to areas that have lost the pigment.
Punch grafting: In this small punches of skin are taken out from the pigmented area and placed over the white patches after making sites for their placement.
Blister Grafting: In this process, multiple small blisters are created in the skin from the donor site in the patient using syringes and suction caps. The top layer of pigmented skin from the blisters are transplanted to the discolored skin area.
NCECS: In this thin layer of pigmented skin is taken out and processed to prepare a cell suspension which is then applied to the prepared recipient white patch area.
Tattooing (Micropigmentation): In this technique artificial pigments are implanted into the skin so that the color of white patch changes and matches the surrounding area.
Decision about which surgery will be suitable for the candidate is taken by the dermatologist after examining the patients patches number, size and site.
Some complications that can occur after a vitiligo surgery are as follows: -
However, the surgeon will take every preventive measure to ensure that the patient gets the best results.
Psoriasis is a non-contagious skin disorder that cause chronic scaly rash on skin. It is caused by dysfunction of the immune system resulting in major turnover of cells. This leads to thickening of skin and raised red colored patches with dry and silvery white scales. It can occur in people of any age group. Although it doesn\'t spread from person to person, it may develop due to a family heredity.
The skin patches may appear anywhere on the body. Some people may also experience scalp, nail and joint involvement. There can be different patterns of skin involvement like Plaque, Guttate, Inverse, Pustular, Erythrodermic
How can you know if you have Psoriasis? Although, the signs and symptoms may vary from person to person, here are some of the usual symptoms:
Plaque: It develops as reddish patches on the skin that may be covered by silvery white coating called scales.
Itching: The patches may develop itching and may get gradually thickened if they are scratched.
Nail problems: Pits, crumbling and falling off nails may be experienced by a few.
Erythrodermic psoriasis: Redness and scaling affecting extensive body surface area.
Pustular psoriasis It may have symptoms such as; red and swollen bumps filled with pus, soreness and pain in areas where erosions occur, problems like fever, chills, severe itching, loss of appetite.
The condition of psoriasis is linked to genetic and environmental components. It is also mediated by the abnormal activity of immune system. To understand the cause of psoriasis, understand the following cycle of skin cells: The skin cells in the deepest layer of skin moves towards the surface in a months time while maturing. During psoriasis, the skin cycle gets rapidly disturbed. So, the cells start moving from the deeper layers of skin to the surface in about 4 days instead of a month not giving enough time to cells to get mature. As a result, it starts accumulating on the surface of skin forming raised, red patches of psoriasis.
Along with genetic combinations, this skin disorder may be precipitated by stressful events, cold and dry weather, trauma like a cut and intake of certain anti-malarial medicines.
This condition can appear in anyone, however, the factors that put you at a higher risk include: Family history of psoriasis, Viral and bacterial infections – such as HIV, strep throat etc, High levels of stress, Overweight, Smoking.
Prevention tips:- Psoriasis is a skin disorder related to abnormal activity of immune system and skin cells, hence, it cannot be completely prevented. However, there are certain ways to control the symptoms:
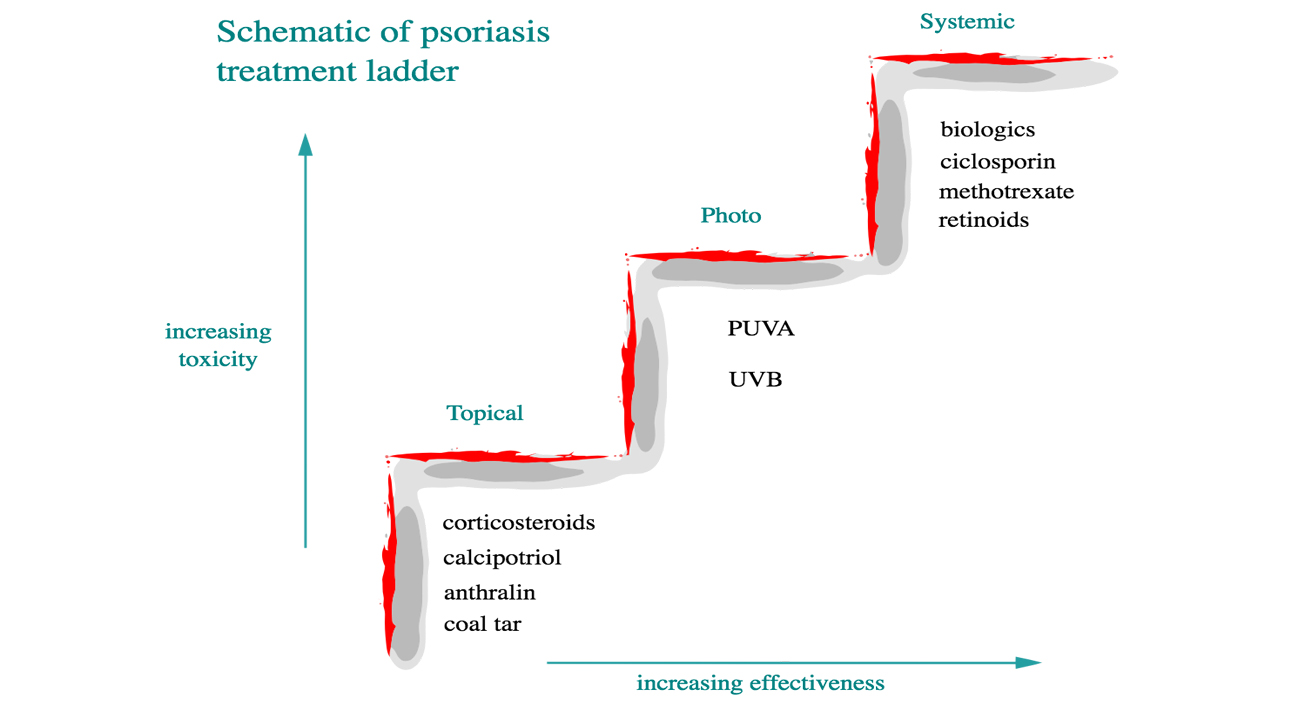
Treatment is guided by diseases severity. For limited disease topical medicines are given and in case of extensive involvement oral drugs and or phototherapy is given.
The type of psoriasis treatment will depend upon your symptoms and your medication history. Seek help of the dermatologist about the options that will work for you and are safe.

